Surgical Procedures
Extractions
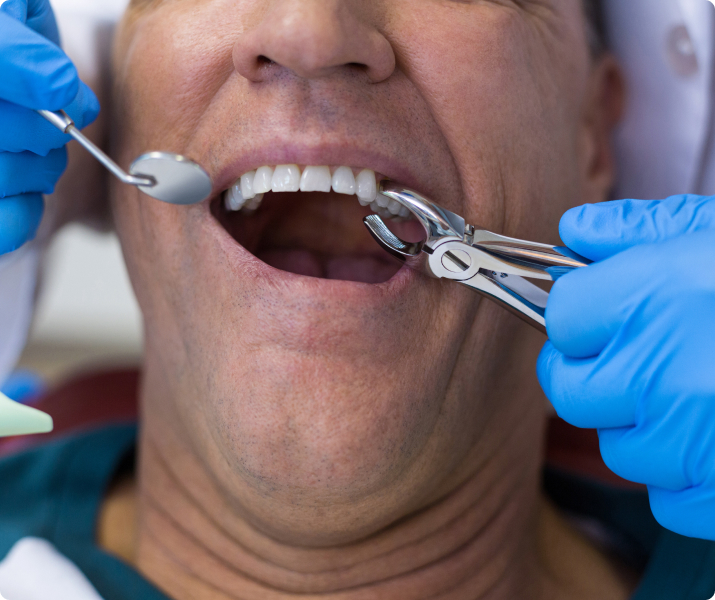
The Extraction Process
If you do feel pain at any time during the extraction, please let us know right away.
After Care
Bleeding
Some bleeding may occur. Placing a piece of gauze over the empty tooth socket and biting down firmly for 30 minutes can control this.
Blood Clots That Form In The Empty Socket
This is an important part of the healing process and you must be careful not to dislodge the clot.
- Avoid rinsing or spitting for 24 hours after the extraction.
- Avoid use of a straw, smoking, drinking hot liquids and alcohol.
Swelling
If swelling occurs, you can place ice on your face for 20 minutes and off for 20 minutes. Repeat this cycle as you feel necessary for up to 24 hours.
Pain & Medications
If you experience pain, you might use non-prescription pain relief medications such as acetaminophen or ibuprofen. Dr. Izadi may also prescribe a stronger medication for you to take if you experience break-through pain.
Eating
For most extractions, make sure you do your chewing away from the extraction site. Stay away from hot liquids and alcoholic beverages for 24 hours. A liquid diet may be recommended for 24 hours.
Brushing & Cleaning
After the extraction, avoid brushing the teeth near the extraction site for one day. After that you can resume gentle cleaning. Avoid commercial mouth rinses containing alcohol, as they tend to irritate the extraction site.
Beginning 24 hours after the extraction, you can rinse with salt water (one teaspoon salt in a cup of warm water) after meals and before bed.
Dry Socket
Dry socket is when a blood clot fails to form in the socket where the tooth has been extracted or the clot has been dislodged and the healing is significantly delayed.
Following the postoperative extraction instructions will reduce the chances of developing dry socket. Dry sockets manifest themselves as a dull throbbing pain that usually doesn’t appear until three to four days after the extraction. The pain can be moderate to severe and radiate from the extraction area. Dry socket may cause a bad taste or bad breath and the extraction site appears dry.
The doctor will apply a medicated dressing to the dry socket to soothe the pain.
Healing
After a tooth has been extracted, there will be a resulting hole in your jawbone where the tooth was. In time, this will smooth and fill in with bone. This process can take many weeks or months. However after 1- 2 weeks you should no longer notice any inconvenience.
Replacing Teeth With
Wisdom Teeth

Why Should I Have My Wisdom Teeth Removed?
Wisdom teeth are the last teeth to erupt within the mouth. When they align properly and gum tissue is healthy, wisdom teeth do not have to be removed. Unfortunately, this does not generally happen. The extraction of wisdom teeth is necessary when they are prevented from properly erupting within the mouth. They may grow sideways, partially emerge from the gum, and even remain trapped beneath the gum and bone. Impacted teeth can take many positions in the bone as they attempt to find a pathway that will allow them to successfully erupt.
These poorly positioned impacted teeth can cause many problems. When they are partially erupted, the opening around the teeth allows bacteria to grow and will eventually cause an infection. The result: swelling, stiffness, pain, and illness. The pressure from the erupting wisdom teeth may move other teeth and disrupt the orthodontic or natural alignment of teeth. The most serious problem occurs when tumors or cysts form around the impacted wisdom teeth, resulting in the destruction of the jawbone and healthy teeth. Removal of the offending impacted teeth usually resolves these problems. Early removal is recommended to avoid such future problems and to decrease the surgical risk involved with the procedure.
Oral Examination
With an oral examination and x-rays of the mouth, Dr. Izadi can evaluate the position of the wisdom teeth and predict if there are present or may be future problems. Studies have shown that early evaluation and treatment result in a superior outcome for the patient. Patients are generally first evaluated in the mid-teenage years by their dentist, orthodontist or by an oral and maxillofacial surgeon.
All outpatient surgery is performed under appropriate anesthesia to maximize patient comfort. Dr. Izadi has the training, license and experience to provide various types of anesthesia for patients to select the best alternative. He is also a diplomate of the American Dental Society of Anesthesiology.
Wisdom Tooth Removal Overview
For a brief narrated overview of the wisdom tooth removal process, please click the image below. It will launch our flash educational MiniModule in a separate window that may answer some of your questions about wisdom teeth.
In most cases, the removal of wisdom teeth is performed under local anesthesia, laughing gas (nitrous oxide/oxygen analgesia) or general anesthesia. These options, as well as the surgical risks (i.e., sensory nerve damage, sinus complications), will be discussed with you before the procedure is performed. Once the teeth are removed, the gum is sutured. To help control bleeding, bite down on the gauze placed in your mouth. You will rest under our supervision in the office until you are ready to be taken home. Upon discharge, your postoperative kit will include postoperative instructions, gauze, a prescription for pain medication, antibiotics, and a follow-up appointment in one week. If you have any questions, please do not hesitate to call us at 540-371-4131.
Our services are provided in an environment of optimum safety that utilizes modern monitoring equipment and staff who are experienced in anesthesia techniques.
Dental Implants

What Are Dental Implants?
Implants also help preserve facial structure, preventing bone deterioration that occurs when teeth are missing.
The Surgical Procedure
For most patients, the placement of dental implants involves two surgical procedures. First, implants are placed within your jawbone. For the first three to six months following surgery, the implants are beneath the surface of the gums gradually bonding with the jawbone. You should be able to wear temporary dentures and eat a soft diet during this time. At the same time, your dentist is fabricating new replacement teeth.
After the implant has bonded to the jawbone, the second phase begins. Dr. Izadi will uncover the implants and attach small posts that protrude through the gums and will act as anchors for the artificial teeth. When the artificial teeth are placed, these posts will not be seen. The entire procedure usually takes six to eight months. Most patients experience minimal disruption in their daily life.
Surgical Advances
Using the most recent advances in dental implant technology, Dr. Izadi is able to place single stage implants. These implants do not require a second procedure to uncover them, but do require a minimum of six weeks of healing time before artificial teeth are placed. There are even situations where the implants can be placed at the same time as a tooth extraction – further minimizing the number of surgical procedures. Advances in dental implant technology have made it possible, in select cases, to extract teeth and place implants with crowns at one visit. This procedure is called “immediate loading”.
Implants are a team effort between an oral and maxillofacial surgeon and a restorative dentist. While Dr. Izadi performs the actual implant surgery, initial tooth extractions, and bone grafting if necessary, the restorative dentist (your dentist) fits and makes the permanent prosthesis. Your dentist will also make any temporary prosthesis needed during the implant process.
What Types Of Prosthesis Are Available?
A single prosthesis (crown) is used to replace one missing tooth – each prosthetic tooth attaches to its own implant. A partial prosthesis (fixed bridge) can replace two or more teeth and may require only two or three implants. A complete dental prosthesis (fixed bridge) replaces all the teeth in your upper or lower jaw. The number of implants varies depending upon which type of complete prosthesis (removable or fixed) is recommended. A removable prosthesis (over denture) attaches to a bar or ball in socket attachments, whereas a fixed prosthesis is permanent and removable only by the dentist. Dr. Izadi will work with your dentist, who will determine which type of prothesis will be best suited for you.
Dr. Izadi performs in-office implant surgery in a hospital-style operating suite, thus optimizing the level of sterility. Inpatient hospital implant surgery is for patients who have special medical or anesthetic needs or for those who need extensive bone grafting from the hip.
Why Select Dental Implants Over More Traditional Types Of Restorations?
There are several reasons: Why sacrifice the structure of surrounding good teeth to bridge a space? In addition, removing a denture or a “partial” at night may be inconvenient, not to mention that dentures that slip can be uncomfortable and rather embarrassing.
Are You A Candidate For Implants?
If you are considering implants, your mouth must be examined thoroughly and your medical and dental history reviewed. If you mouth is not ideal for implants, ways of improving outcome, such as bone grafting, may be recommended.
What Type Of Anesthesia Is Used?
The majority of dental implants and bone grafts can be performed in the office under local anesthesia, with or without general anesthesia.
Do Implants Need Special Care?
Sinus Lift Procedure
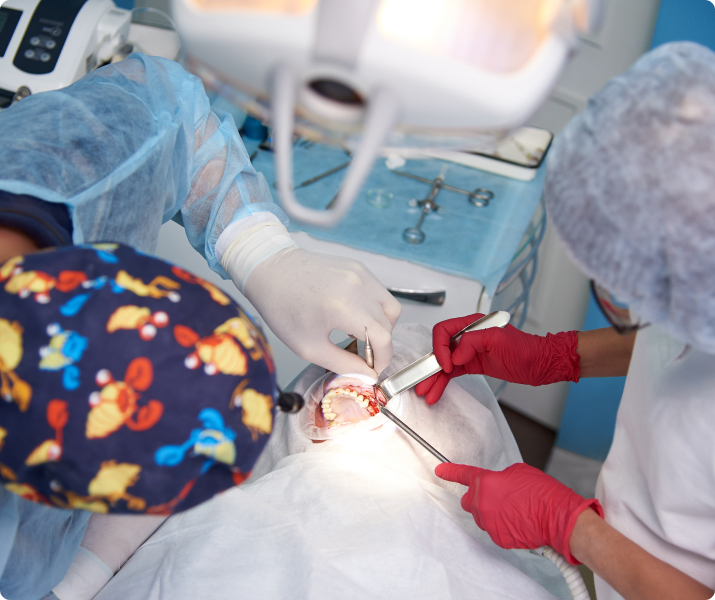
Sinus Lift Procedure
The maxillary sinuses are behind your cheeks and on top of the upper teeth. Sinuses are like empty rooms that have nothing in them. Some of the roots of the natural upper teeth extend up into the maxillary sinuses. When these upper teeth are removed, there is often just a thin wall of bone separating the maxillary sinus and the mouth. Dental implants need bone to hold them in place. When the sinus wall is very thin, it is impossible to place dental implants in this bone.
The solution to this is called a sinus graft or sinus lift. The dental implant surgeon enters the sinus from where the upper teeth used to be. The sinus membrane is then lifted upward and donor bone is inserted into the floor of the sinus. Keep in mind that the floor of the sinus is the roof of the upper jaw. After several months of healing, the bone becomes part of the patient’s jaw and dental implants can be inserted and stabilized in this new sinus bone.
The sinus graft makes it possible for many patients to have dental implants when years ago there was no other option other than wearing loose dentures.
If enough bone between the upper jaw ridge and the bottom of the sinus is available to stabilize the implant well, sinus augmentation and implant placement can sometimes be performed as a single procedure. This technique is called an indirect sinus lift.
If not enough bone is available, the sinus augmentation will have to be performed first, then the graft will have to mature for several months, depending upon the type of graft material used. Once the graft has matured, the implants can be placed.
Bone Grafting
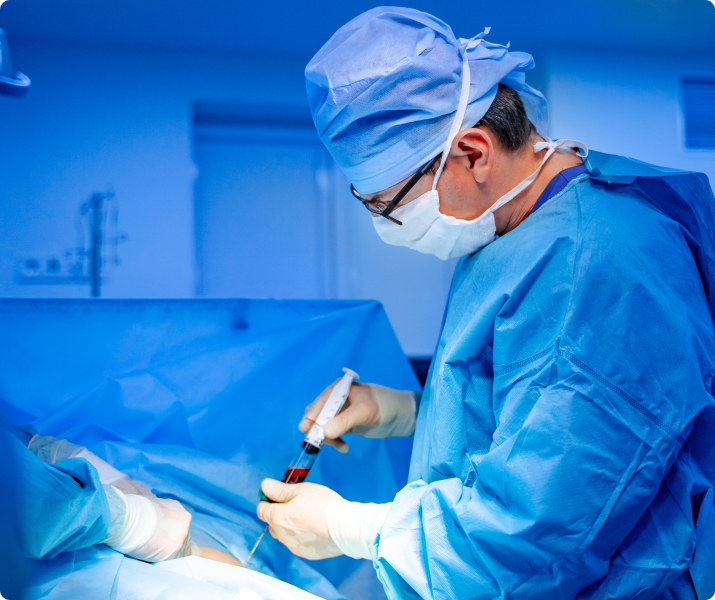
Major & Minor Bone Grafting
Over a period of time, the jawbone associated with missing teeth atrophies, or is reabsorbed. This often leaves a condition in which there is poor quality and quantity of bone suitable for placement of dental implants. In these situations, most patients are not candidates for placement of dental implants.
Today, we have the ability to grow bone where needed. This not only gives us the opportunity to place implants of proper length and width, it also gives us a chance to restore functionality and aesthetic appearance.
Major Bone Grafting
Bone grafting can repair implant sites with inadequate bone structure due to previous extractions, gum disease or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw, hip or tibia (below the knee). Sinus bone grafts are also performed to replace bone in the posterior upper jaw. In addition, special membranes may be utilized that dissolve under the gum and protect the bone graft and encourage bone regeneration. This is called guided bone regeneration or guided tissue regeneration.
Major bone grafts are typically performed to repair defects of the jaws. These defects may arise as a result of traumatic injuries, tumor surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different sites depending on the size of the defect. The skull (cranium), hip (iliac crest), and lateral knee (tibia), are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay.
Ridge Expansion
In severe cases, the ridge has been resorbed and a bone graft is placed to increase ridge height and/or width. This is a technique used to restore the lost bone dimension when the jaw ridge gets too thin to place conventional implants. In this procedure, the bony ridge of the jaw is literally expanded by mechanical means. Bone graft material can be placed and matured for a few months before placing the implant.
Nerve Repositioning
The inferior alveolar nerve, which gives feeling to the lower lip and chin, may need to be moved in order to make room for placement of dental implants in the lower jaw. This procedure is limited to the lower jaw and indicated when teeth are missing in the area of the two back molars and/or second premolar, with the above-mentioned secondary condition. Since this procedure is considered a very aggressive approach (there is almost always some postoperative numbness of the lower lip and jaw area, which dissipates only very slowly, if ever), usually other, less aggressive options are considered first (bone grafts or placement of blade implants, etc.).
Typically, an outer section of the cheek side of the lower jawbone is removed in order to expose the nerve and vessel canal. Then we isolate the nerve and vessel bundle in that area and slightly pull it out to the side. At the same time, we will place the implants. Then the bundle is released and placed back over the implants. The surgical access is refilled with bone graft material of the surgeon’s choice and the area is closed.
These procedures may be performed separately or together, depending upon the individual’s condition. As stated earlier, there are several areas of the body that are suitable for attaining bone grafts. In the maxillofacial region, bone grafts can be taken from inside the mouth, in the area of the chin or third molar region, or in the upper jaw behind the last tooth. In more extensive situations, a greater quantity of bone can be attained from the hip or the outer aspect of the tibia at the knee. When we use the patient’s own bone for repairs, we generally get the best results.
In many cases, we can use allograft material to implement bone grafting for dental implants. This bone is prepared from cadavers and used to promote the patients own bone to grow into the repair site. It is quite effective and very safe. Synthetic materials can also be used to stimulate bone formation. We even use factors from your own blood to accelerate and promote bone formation in graft areas.
These surgeries are performed in the surgical suite at the office under IV sedation or general anesthesia. After discharge, bed rest is recommended for one day and limited physical activity for one week.
Impacted Canines
An impacted tooth simply means that it is “stuck” and cannot erupt into function. Patients frequently develop problems with impacted third molar (wisdom) teeth. These teeth get “stuck” in the back of the jaw and can develop painful infections among a host of other problems. Since there is rarely a functional need for wisdom teeth, they are usually extracted if they develop problems. The maxillary cuspid (upper eyetooth) is the second most common tooth to become impacted. The cuspid tooth is a critical tooth in the dental arch and plays an important role in your “bite”. The cuspid teeth are very strong biting teeth and have the longest roots of any human teeth. They are designed to be the first teeth that touch when your jaws close together so they guide the rest of the teeth into the proper bite.
Normally, the maxillary cuspid teeth are the last of the “front” teeth to erupt into place. They usually come into place around age 13 and cause any space left between the upper front teeth to close tighter together. If a cuspid tooth gets impacted, every effort is made to get it to erupt into its proper position in the dental arch. The techniques involved to aid eruption can be applied to any impacted tooth in the upper or lower jaw, but most commonly they are applied to the maxillary cuspid (upper eye) teeth. Sixty percent of these impacted eyeteeth are located on the palatal (roof of the mouth) side of the dental arch. The remaining impacted eye teeth are found in the middle of the supporting bone but stuck in an elevated position above the roots of the adjacent teeth or out to the facial side of the dental arch.
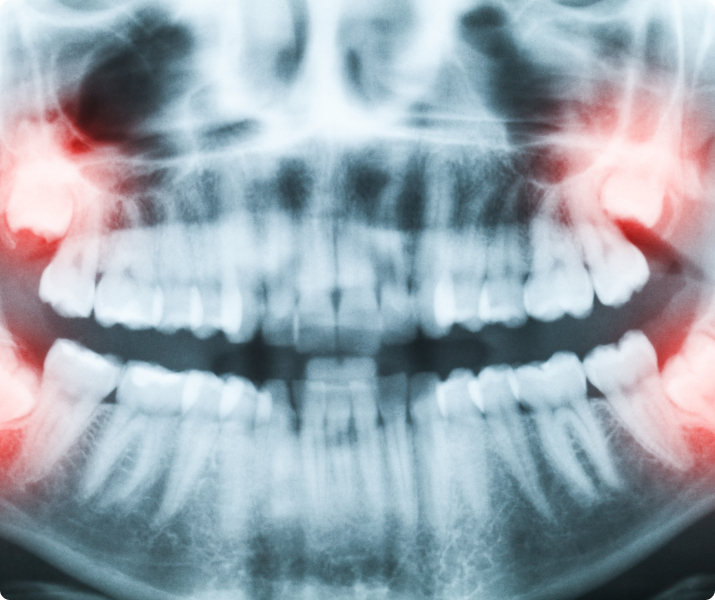
What Happens If The Canine Will Not Erupt When Proper Space Is Available?
In cases where the eyeteeth will not erupt spontaneously, the orthodontist and oral surgeon work together to get these unerupted eyeteeth to erupt. Each case must be evaluated on an individual basis but treatment will usually involve a combined effort between the orthodontist and the oral surgeon. The most common scenario will call for the orthodontist to place braces on the teeth (at least the upper arch). A space will be opened to provide room for the impacted tooth to be moved into its proper position in the dental arch. If the baby eyetooth has not fallen out already, it is usually left in place until the space for the adult eyetooth is ready. Once the space is ready, the orthodontist will refer the patient to the oral surgeon to have the impacted eyetooth exposed and bracketed.
In a simple surgical procedure performed in the surgeon’s office, the gum on top of the impacted tooth will be lifted up to expose the hidden tooth underneath. If there is a baby tooth present, it will be removed at the same time. Once the tooth is exposed, the oral surgeon will bond an orthodontic bracket to the exposed tooth. The bracket will have a miniature gold chain attached to it. The oral surgeon will guide the chain back to the orthodontic arch wire where it will be temporarily attached. Sometimes the surgeon will leave the exposed impacted tooth completely uncovered by suturing the gum up high above the tooth or making a window in the gum covering the tooth (on selected cases located on the roof of the mouth). Most of the time, the gum will be returned to its original location and sutured back with only the chain remaining visible as it exits a small hole in the gum.
Shortly after surgery (1-14 days) the patient will return to the orthodontist. A rubber band will be attached to the chain to put a light eruptive pulling force on the impacted tooth. This will begin the process of moving the tooth into its proper place in the dental arch. This is a carefully controlled, slow process that may take up to a full year to complete. Remember, the goal is to erupt the impacted tooth and not to extract it! Once the tooth is moved into the arch in its final position, the gum around it will be evaluated to make sure it is sufficiently strong and healthy to last for a lifetime of chewing and tooth brushing. In some circumstances, especially those where the tooth had to be moved a long distance, there may be some minor “gum surgery” required to add bulk to the gum tissue over the relocated tooth so it remains healthy during normal function. Your dentist or orthodontist will explain this situation to you if it applies to your specific situation.
These basic principals can be adapted to apply to any impacted tooth in the mouth. It is not that uncommon for both of the maxillary cuspids to be impacted. In these cases, the space in the dental arch form will be prepared on both sides at once. When the orthodontist is ready, the surgeon will expose and bracket both teeth in the same visit so the patient only has to heal from surgery once. Because the anterior teeth (incisors and cuspids) and the bicuspid teeth are small and have single roots, they are easier to erupt if they get impacted than the posterior molar teeth. The molar teeth are much bigger teeth and have multiple roots making them more difficult to move. The orthodontic maneuvers needed to manipulate an impacted molar tooth can be more complicated because of their location in the back of the dental arch.
Recent studies have revealed that with early identification of impacted eyeteeth (or any other impacted tooth other than wisdom teeth), treatment should be initiated at a younger age. Once the general dentist or hygienist identifies a potential eruption problem, the patient should be referred to the orthodontist for early evaluation. In some cases the patient will be sent to the oral surgeon before braces are even applied to the teeth. As mentioned earlier, the surgeon will be asked to remove over-retained baby teeth and/or selected adult teeth. He will also remove any extra teeth or growths that are blocking eruption of the developing adult teeth. Finally, he may be asked to simply expose an impacted eyetooth without attaching a bracket and chain to it. In reality, this is an easier surgical procedure to perform than having to expose and bracket the impacted tooth. This will encourage some eruption to occur before the tooth becomes totally impacted (stuck). By the time the patient is at the proper age for the orthodontist to apply braces to the dental arch, the eyetooth will have erupted enough that the orthodontist can bond a bracket to it and move it into place without needing to force its eruption. In the long run, this saves time for the patient and means less time in braces (always a plus for any patient!).
What To Expect From Surgery To Expose & Bracket An Impacted Tooth?
The surgery to expose and bracket an impacted tooth is a very straightforward surgical procedure that is performed in the oral surgeon’s office. For most patients, it is performed under IV sedation and/or General Anesthesia. In some selected cases it will be performed under local anesthesia. The procedure is generally scheduled for 45 minutes if one tooth is being exposed and bracketed and 60 minutes if both sides require treatment. If the procedure only requires exposing the tooth with no bracketing, the time required will be shortened by about one half. These issues will be discussed in detail at your preoperative consultation with your doctor. You can also refer to Preoperative Instructions under Surgical Instructions on this website for a review of any details.
You can expect a limited amount of bleeding from the surgical sites after surgery. Although there will be some discomfort after surgery at the surgical sites, most patients find Tylenol or Advil to be more than adequate to manage any pain they may have. Within two to three days after surgery there is usually little need for any medication at all. There may be some swelling from holding the lip up to visualize the surgical site; it can be minimized by applying ice packs to the lip for the afternoon after surgery. Bruising is not a common finding at all after these cases. A soft, bland diet is recommended at first, but you may resume your normal diet as soon as you feel comfortable chewing. It is advised that you avoid sharp food items like crackers and chips as they will irritate the surgical site if they jab the wound during initial healing. Your doctor will see you seven to ten days after surgery to evaluate the healing process and make sure you are maintaining good oral hygiene. You should plan to see your orthodontist within 1-14 days to activate the eruption process by applying the proper rubber band to the chain on your tooth. As always your doctor is available at the office or can be reached after hours if any problems should arise after surgery. Simply call Fredericksburg Implant and Oral Surgery Associates at 540-371-4131 if you have any questions.
Platelet Rich Plasma

Why All The Excitement About PRP?
PRP permits the body to take advantage of the normal healing pathways at a greatly accelerated rate. During the healing process, the body rushes many cells and cell-types to the wound in order to initiate the healing process. One of those cell types is platelets. Platelets perform many functions, including formation of a blood clot and release of growth factors (GF) into the wound. These GF (platelet derived growth factors PGDF, transforming growth factor beta TGF, and insulin-like growth factor ILGF) function to assist the body in repairing itself by stimulating stem cells to regenerate new tissue. The more growth factors released sequestered into the wound, the more stem cells stimulated to produce new host tissue. Thus, one can easily see that PRP permits the body to heal faster and more efficiently.
A subfamily of TGF, is bone morphogenic protein (BMP). BMP has been shown to induce the formation of new bone in research studies in animals and humans. This is of great significance to the surgeon who places dental implants. By adding PRP, and thus BMP, to the implant site with bone substitute particles, the implant surgeon can now grow bone more predictably and faster than ever before.
PRP Has Many Clinical Applications
- Bone grafting for dental implants. This includes onlay and inlay grafts, sinus lift procedures, ridge augmentation procedures, and closure of cleft, lip, and palate defects.
- Repair of bone defects creating by removal of teeth or small cysts.
- Repair of fistulas between the sinus cavity and mouth.
PRP Also Has Many Advantages
Safety: PRP is a by-product of the patient’s own blood, therefore, disease transmission is not an issue.
Convenience: PRP can be generated in the doctor’s office while the patient is undergoing an outpatient surgical procedure, such as placement of dental implants.
Faster healing: The supersaturation of the wound with PRP, and thus growth factors, produces an increase of tissue synthesis and thus faster tissue regeneration.
Cost effectiveness: Since PRP harvesting is done with only a small amount of blood in the doctor’s office, the patient need not incur the extremely high expense of the harvesting procedure in the hospital or at the blood bank.
Ease of use: PRP is easy to handle and actually improves the ease of application of bone substitute materials and bone grafting products by making them more gel-like.
Frequently Asked Questions About PRP
Is PRP safe? Yes. During the outpatient surgical procedure a small amount of your own blood is drawn out via the IV. This blood is then placed in the PRP centrifuge machine and spun down. In less than 15 minutes, the PRP is formed and ready to use.
Should PRP be used in all bone-grafting cases? Not always. In some cases, there is no need for PRP. However, in the majority of cases, application of PRP to the graft will increase the final amount of bone present in addition to making the wound heal faster and more efficiently.
Will my insurance cover the costs?Unfortunately not. The cost of the PRP application is paid by the patient.
Can PRP be used alone to stimulate bone formation? No. PRP must be mixed with either the patient’s own bone, a bone substitute material such as demineralized freeze-dried bone, or a synthetic bone product, such as BIO-OSS.
Are there any contraindications to PRP?Very few. Obviously, patients with bleeding disorders or hematologic diseases do not qualify for this in-office procedure. Check with your surgeon and/or primary care physician to determine if PRP is right for you.
Facial Trauma
Dr. Izadi is trained, skilled, and uniquely qualified to manage and treat facial trauma. These injuries include:
- Facial lacerations
- Intra oral lacerations
- Avulsed (knocked out) teeth
- Fractured facial bones (cheek, nose or eye socket)
- Fractured jaws (upper and lower jaw)
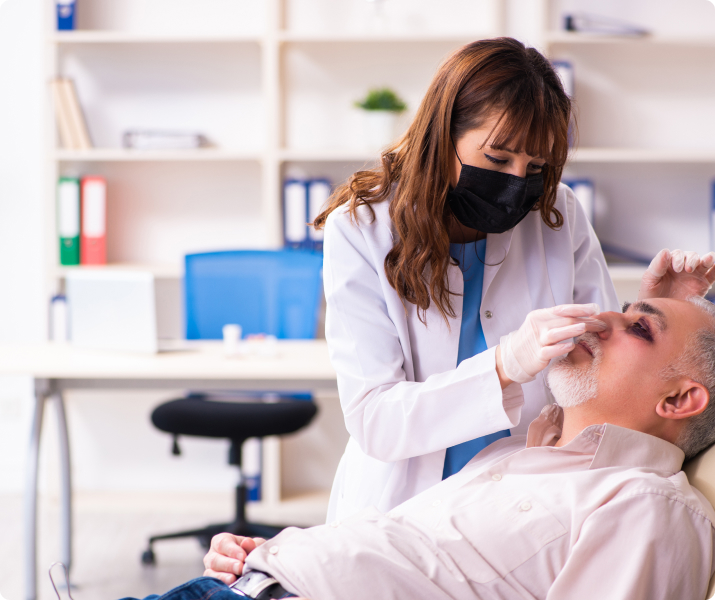
The Nature Of Maxillofacial Trauma
There are a number of possible causes of facial trauma such as motor vehicle accidents, accidental falls, sports injuries, interpersonal violence, and work-related injuries. Types of facial injuries can range from injuries of teeth to extremely severe injuries of the skin and bones of the face. Typically, facial injuries are classified as either soft tissue injuries (skin and gums), bone injuries (fractures), or injuries to special regions (such as the eyes, facial nerves or the salivary glands).
Soft Tissue Injuries Of The Maxillofacial Region
When soft tissue injuries such as lacerations occur on the face, they are repaired by suturing. In addition to the obvious concern of providing a repair that yields the best cosmetic result possible, care is taken to inspect for and treat injuries to structures such as facial nerves, salivary glands, and salivary ducts (or outflow channels). Dr. Izadi is a well-trained oral and maxillofacial surgeon and is proficient at diagnosing and treating all types of facial lacerations.
Bone Injuries Of The Maxillofacial Region
Fractures of the bones of the face are treated in a manner similar to the fractures in other parts of the body. The specific form of treatment is determined by various factors, which include the location of the fracture, the severity of the fracture, the age, and general health of the patient. When an arm or a leg is fractured, a cast is often applied to stabilize the bone to allow for proper healing. Since a cast cannot be placed on the face, other means have been developed to stabilize facial fractures.
One of these options involves wiring the jaws together for certain fractures of the upper and/or lower jaw. Certain other types of fractures of the jaw are best treated and stabilized by the surgical placement of small plates and screws at the involved site. This technique of treatment can often allow for healing and obviates the necessity of having the jaws wired together. This technique is called “rigid fixation” of a fracture. The relatively recent development and use of rigid fixation has profoundly improved the recovery period for many patients, allowing them to return to normal function more quickly.
The treatment of facial fractures should be accomplished in a thorough and predictable manner. More importantly, the patient’s facial appearance should be minimally affected. An attempt at accessing the facial bones through the fewest incisions necessary is always made. At the same time, the incisions that become necessary, are designed to be small and, whenever possible, are placed so that the resultant scar is hidden.
Injuries To The Teeth & Surrounding Dental Structures
Isolated injuries to teeth are quite common and may require the expertise of various dental specialists. Oral surgeons usually are involved in treating fractures in the supporting bone or in replanting teeth that have been displaced or knocked out. These types of injuries are treated by one of a number of forms of splinting (stabilizing by wiring or bonding teeth together). If a tooth is knocked out, it should be placed in salt water or milk. The sooner the tooth is re-inserted into the dental socket, the better chance it will survive. Therefore, the patient should see a dentist or oral surgeon as soon as possible. Never attempt to wipe the tooth off, since remnants of the ligament that hold the tooth in the jaw are attached and are vital to the success of replanting the tooth. Other dental specialists may be called upon such as endodontists, who may be asked to perform root canal therapy, and/or restorative dentists who may need to repair or rebuild fractured teeth. In the event that injured teeth cannot be saved or repaired, dental implants are often now utilized as replacements for missing teeth.
Oral Pathology
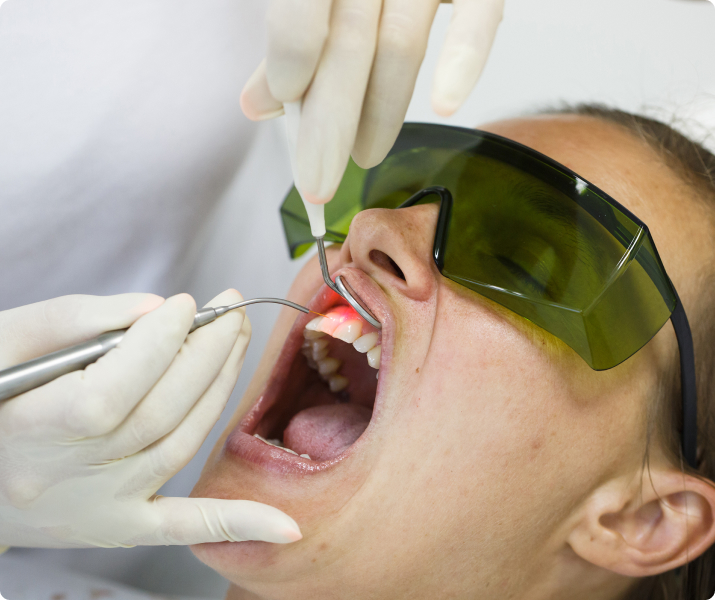
Oral Pathology
The inside of the mouth is normally lined with a special type of skin (mucosa) that is smooth and coral pink in color. Any alteration in this appearance could be a warning sign for a pathological process. The most serious of these is oral cancer. The following can be signs at the beginning of a pathologic process or cancerous growth:
- Reddish patches (erythroplasia) or whitish patches (leukoplakia) in the mouth
- A sore that fails to heal and bleeds easily
- A lump or thickening on the skin lining the inside of the mouth
- Chronic sore throat or hoarseness
- Difficulty in chewing or swallowin
These changes can be detected on the lips, cheeks, palate and gum tissue around the teeth, tongue, face and/or neck. Pain does not always occur with pathology, and curiously, is not often associated with oral cancer. However, any patient with facial and/or oral pain without an obvious cause or reason may also be at risk for oral cancer.
We would recommend performing an oral cancer self-examination monthly and remember that your mouth is one of your body’s most important warning systems. Do not ignore suspicious lumps or sores. Please contact us so we may help.